Silver diamine fluoride (SDF) 38% is a concentrated, liquid topical treatment that helps arrest active dental decay without drilling. Originally developed for treating tooth sensitivity, clinicians discovered its ability to halt the progression of cavities by combining the antibacterial action of silver with the remineralizing effects of fluoride. Because it is applied directly to the affected tooth surface and does not require injections or removal of tooth structure, SDF can be an excellent choice for young children and others who have difficulty sitting through longer procedures.
In practice, SDF works by penetrating softened enamel and dentin, creating an environment that is less favorable to the bacteria responsible for decay. The treated area becomes harder and less likely to progress, which buys time for monitoring, improved home care, or future restorative treatment when appropriate. While it does not replace restorative dentistry in every case, SDF is an evidence-based tool that expands the options available to families seeking conservative, trauma-free care.
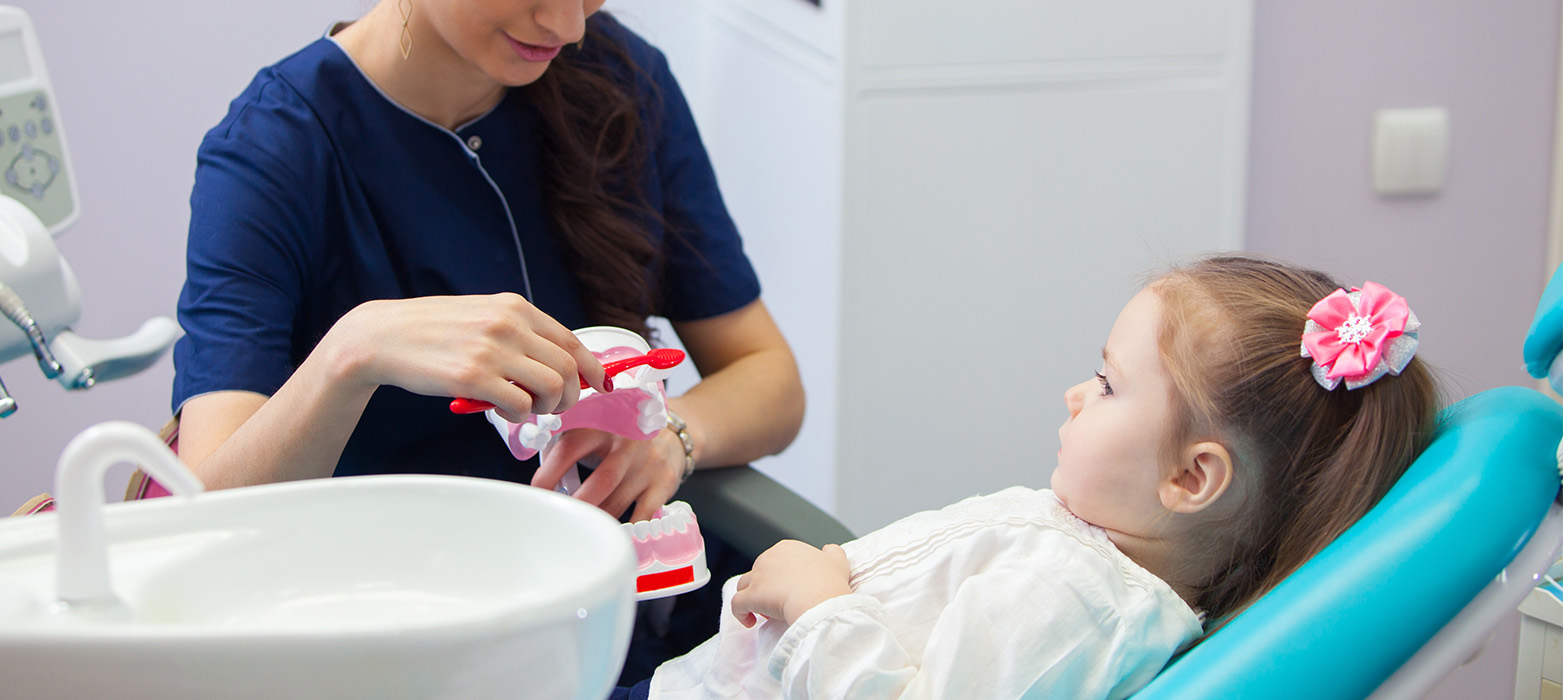
Because SDF is a topical liquid, applications are quick and painless: the affected surface is cleaned and dried, a small amount of SDF is applied with a microbrush, and the area is allowed to dry. The simplicity of this approach makes it particularly useful for very young patients, children with special needs, and anyone for whom traditional operative treatment is not feasible at the moment.
Deciding whether silver diamine fluoride is appropriate starts with a careful clinical exam and a conversation about goals. SDF is most often recommended for small, active carious lesions, for initial management of decay on primary (baby) teeth, or as a stopgap when immediate restoration isn’t possible. It is also a practical option for patients who experience dental anxiety, have medical conditions that complicate longer visits, or for whom behavioral management is a concern.
Clinicians will assess factors such as lesion size and location, the child’s cooperative ability, and the family’s preferences before recommending SDF. One important aesthetic consideration is that SDF typically darkens the treated decay; while this discoloration signals that the lesion has been arrested, families should be informed of the visual change in advance so expectations are clear. For some teeth and situations, alternative or follow-up restorative work may still be recommended.
Because it is minimally invasive and can be repeated as needed, SDF often becomes part of a staged treatment plan—used to stabilize disease, reduce pain or infection risk, and create a calmer setting for future care. This patient-centered approach allows clinicians to prioritize comfort and safety while still addressing oral health needs effectively.
Silver diamine fluoride is most effective when used alongside other preventive measures rather than as a stand-alone solution. Routine dental exams, professional cleanings, fluoride varnish applications, and dental sealants all play complementary roles in reducing decay risk. SDF can be introduced as one tool among many to manage disease and support long-term oral health for children.
During regular visits, dental professionals perform risk assessments that guide individualized prevention plans. For children at higher risk of caries, those plans often include more frequent monitoring, tailored fluoride strategies, dietary guidance, and targeted preventive interventions like SDF or sealants. The combination of in-office care and consistent at-home routines produces the strongest protection against future cavities.
Importantly, preventive dentistry is dynamic; treatment choices evolve as a child grows, their oral environment changes, and their ability to cooperate improves. Using minimally invasive options such as SDF early on can reduce the need for more invasive procedures later and supports a positive experience that encourages lifelong oral care habits.
Preventing cavities is a team effort that continues at home. Caregivers and older children can reinforce the benefits of in-office treatments by maintaining good daily habits: brushing twice a day with a fluoride toothpaste, flossing where appropriate, and limiting frequent exposure to sugary or acidic snacks and drinks. These simple routines reduce the bacterial fuel that drives decay and make professional interventions more effective.
For very young children, using an appropriate smear or pea-sized amount of fluoride toothpaste and supervising brushing until they can reliably spit are important steps. Establishing regular meal and snack patterns and encouraging water between meals can also help keep oral pH balanced and reduce decay risk. When a child has received SDF or other preventive treatments, caregivers should continue to follow the home-care guidance provided by the dental team to preserve and extend the benefits of those interventions.
Education and behavior modeling play a major role as well. Teaching children why we brush, making oral hygiene a positive habit, and involving them in simple choices—like selecting a child-friendly toothbrush or a flavored toothpaste—can increase cooperation and make preventive care more effective over time.
After applying SDF or initiating any preventive protocol, follow-up is essential. Regular recall visits allow the dental team to re-evaluate treated areas, repeat applications if needed, and determine whether restorative treatment becomes necessary as a child matures. These checkups also give clinicians the chance to reinforce home-care techniques and adjust recommendations according to the child’s developing needs.
For many families, using SDF as part of a broader prevention strategy helps avoid emergency situations and maintain comfort while preserving tooth structure. When restorative treatment becomes possible or desirable, the practice can coordinate those services while keeping the child’s previous care and tolerance in mind. Continuity and clear communication between families and the dental team help ensure favorable outcomes over the long term.
At Children's Dentistry of Morristown, our goal is to offer preventive solutions that are evidence-based, patient-centered, and respectful of each child’s comfort and circumstances. By combining in-office options like SDF with a strong emphasis on education and daily habits, we aim to protect young smiles and set the foundation for lifelong oral health.
In summary, preventive dental care blends clinical techniques and home practices to stop decay before it progresses. Minimally invasive treatments such as silver diamine fluoride 38% expand the ways clinicians can protect teeth—especially for children and patients who need gentler approaches. Contact us to learn more about preventive options and how we can help you create a customized plan for your child’s oral health.
Silver diamine fluoride, commonly called SDF, is a topical dental liquid used to arrest active tooth decay and help prevent its progression. The formulation most often used in pediatric care is SDF 38%, which combines the antibacterial properties of silver with the remineralizing action of fluoride. Because it is applied directly to decayed surfaces without drilling or injections, SDF offers a minimally invasive alternative for managing early or small lesions.
SDF is not a replacement for all restorative work, but it expands the options available to clinicians and families who seek conservative, trauma-free approaches. It is particularly useful for very young children, those with special healthcare needs, and patients who cannot tolerate longer procedures at the moment. Treatment decisions are individualized based on the child’s clinical presentation and the family’s goals for care.
SDF works through two main actions: the silver component provides broad antibacterial activity that reduces the bacterial load in a lesion, while the fluoride promotes remineralization of weakened enamel and dentin. When applied, the solution penetrates softened tooth structure and creates an environment that is less hospitable to cariogenic bacteria. The combination of bacterial suppression and mineral uptake helps harden the treated area and halt lesion progression.
Over time, the arrested lesion becomes more resistant to further breakdown, which allows clinicians to monitor the site and determine whether additional interventions are needed. Because SDF does not remove decayed tissue, follow-up assessments are essential to confirm stability. In many cases, SDF buys time for improved home care, behavioral management, or later restorative treatment when appropriate.
Candidates for SDF typically include children with small, active cavities, especially on primary (baby) teeth, as well as patients who have difficulty tolerating conventional dental procedures. It is also a practical option for children with dental anxiety, limited cooperation, or medical conditions that make longer visits risky or impractical. Clinicians consider lesion size, location, the child’s behavior, and the family’s preferences when recommending SDF.
SDF is often used as part of a staged treatment plan to stabilize disease and reduce the risk of pain or infection while planning definitive care. For certain teeth or clinical situations, follow-up restorative treatment may still be recommended once the child can tolerate it. A thorough clinical exam and discussion with the dental team will determine whether SDF is appropriate for a given child.
One predictable effect of SDF is that treated areas of decay usually darken to a brown or black color, which indicates that the lesion has been arrested. This change in appearance is a sign that the bacteria have been controlled and the tissue has hardened, but it can be a cosmetic concern depending on the tooth involved and its visibility. Parents should be informed in advance so they understand the trade-off between appearance and the benefits of arresting decay without invasive treatment.
For visible front teeth or other esthetic concerns, clinicians may discuss alternative strategies such as using SDF only on less visible surfaces, applying it as a temporary measure followed by restorative coverage, or choosing other treatment modalities. The dental team will work with families to balance clinical effectiveness and appearance when planning care for each child.
SDF application is a simple, quick procedure that typically requires only a clean, dry tooth surface and basic isolation to protect surrounding tissues. The clinician will gently clean and dry the affected area, isolate it with cotton or other barriers, and then apply a small amount of SDF with a microbrush. The solution is left to absorb and dry for a short period, and the child can leave the office once the area has set.
The minimal nature of the application means there are no injections and no drilling, which reduces stress for many young patients. Applications generally take only a few minutes and can be repeated as needed during recall visits. The dental team will explain the procedure step by step and answer any questions before beginning.
SDF is generally painless to apply and does not require local anesthesia because the procedure does not involve excavation of tooth structure. Most children tolerate the brief application very well, and the quick, noninvasive workflow helps minimize anxiety and movement. Parents should be aware that there can be a temporary metallic taste when SDF is applied, but this typically fades quickly.
In some cases where a child is particularly sensitive or uncooperative, the dental team may use behavioral techniques, distraction, or other supportive measures to increase comfort and cooperation. The goal is to provide effective care while keeping the experience as calm and positive as possible for both child and family.
SDF arrests decay but does not permanently restore lost tooth structure, so its effects are monitored over time and reapplication may be recommended. Clinical studies and practice protocols vary, but many clinicians perform periodic reassessments and apply additional SDF at recall visits if signs of active decay persist. Regular monitoring allows the dental team to determine whether the lesion remains stable or if further restorative care is needed.
The durability of SDF also depends on the child’s oral environment and home-care habits, so combining in-office treatments with consistent brushing, fluoride use, and dietary management strengthens long-term outcomes. If restorative treatment becomes feasible later, the team can plan appropriate follow-up while considering the child’s tolerance and clinical needs.
Yes. SDF is often incorporated into a broader preventive and restorative plan rather than being used in isolation. It can be applied as an interim measure before definitive restorations such as fillings or stainless steel crowns, and it complements other preventive therapies like fluoride varnish and dental sealants. Using SDF as part of a staged approach allows clinicians to manage disease while planning restorative care when appropriate.
In some cases, SDF-treated surfaces can later receive esthetic or full-coverage restorations to address appearance or function once the child is ready. The dental team will outline recommended next steps and coordinate care to ensure continuity and the best long-term result for the child’s oral health.
SDF has a strong safety record when used as directed, but there are a few considerations parents should know. The most common effect is dark staining of treated decay, which is an expected outcome rather than a harmful side effect. Rarely, soft tissue irritation can occur if the solution contacts the gums, and a small metallic taste may be noticeable during application.
Allergic reactions to silver are uncommon but possible, so clinicians review medical and allergy histories before treatment and discuss any concerns with caregivers. Because SDF is applied topically in very small quantities, systemic exposure is minimal; nevertheless, the dental team follows established guidelines to ensure safe, effective use for each patient.
After SDF application, families should continue standard home-care measures such as twice-daily brushing with fluoride toothpaste, appropriate supervision for young children, and limiting frequent sugary snacks and drinks. These daily habits reduce the bacterial fuel for decay and support the benefits achieved with in-office treatments. The dental team will provide specific instructions tailored to the child’s age and risk profile.
Follow-up visits are important to reassess treated areas, determine whether additional SDF applications are needed, and plan any necessary restorative work as the child grows. At Children's Dentistry of Morristown we emphasize clear communication and individualized recall schedules so families understand next steps and feel confident in their child’s preventive care plan.
Phone: